Synopsis: The infection risk associated with heater-cooler devices may be broader in scope and higher than federal health officials have publicly acknowledged. Not just one model, but most heater-cooler devices may become contaminated with mycobacteria, including M. chimaera andM. abscessus (and possibly other types of microorganisms too, including Legionella), published data reveal. The infections linked to these devices appear to be due, often, to intrinsic contamination of one model during manufacturing, or to tap water.
Note: Dr. Muscarella is accepting new clients seeking guidance in infection prevention, hospital infections, instrument reprocessing, and other related topics.
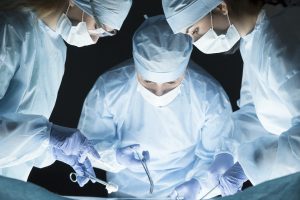
January 18, 2017 (By Lawrence F Muscarella, PhD) — More than one brand of a specialized type of medical equipment used during open-chest surgery has been linked to potentially life-threatening bacterial infections, my research has found.
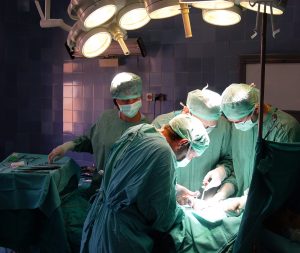
In all, as many as one million U.S. patients since 2011 who underwent the surgery on cardiopulmonary bypass could be at risk of infection. This number rises even more significantly when patients in Europe and other countries using the same equipment are also counted.
More than a year ago, in Oct. 2015, both the FDA and Centers for Disease Control and Prevention began alerting hospitals and healthcare providers about the risk of heater-cooler devices exposing patients to the deadly bacteria.
These alerts were general and did not identify any one particular heater-cooler model, or type of mycobacteria, as posing the infection risk. The recommendations provided in the FDA’s alert applied to “all heater-cooler devices.”
Similarly, the CDC’s alert did not identify a specific model or mycobacteria as posing the risk, stating more broadly that, “this CDC communication is to raise awareness … of the possible association between NTM infections and use of heater-cooler devices and to provide guidance on identifying patients with infection.”
Nor did either alert single-out a likely cause for these infections.
Like the FDA, the CDC would not warn patients (and again healthcare providers) of this infection risk until months later, in June and Oct. 2016, when the CDC advised that “it is imperative that patients and providers are informed about the risk of infection associated with use of (one specific heater-cooler model).”
Heater-cooler devices warm and cool the temperature of the patient’s blood during heart valve repair and replacements, heart and heart-lung transplantation, and the repair of congenital heart abnormalities, among other types of open-chest surgeries.
The 2016 federal alerts: A change in focus
A year after their initial alerts, however, the FDA and CDC each issued updated safety notices, on Oct. 13, 2016, that warned hospitals and open-chest surgery patients about the infection risk associated with these devices.
Among other more recent outbreaks that prompted the FDA and CDC in Oct. 2016 to warn the public about this infection risk, an investigation performed in June 2014, involving both federal and South Carolina health officials, linked as many as fifteen mycobacterial infections and four death to the use of a contaminated heater-cooler device. This outbreak was the first in the U.S. to be publicly linked to a contaminated heater-cooler device.
The FDA’s alert last Oct., however, was noticeably more focused (compared to its safety alert issued the previous year), appearing to limit its scope this time to one heater-cooler model, one specific type of non-tuberculous mycobacteria, or “NTM,” and one possible cause.
Namely, this FDA alert singled out the Stöckert (or, Sorin) 3T Heater-Cooler (LivaNova PLC, Italy, formerly the Sorin Group) as posing an infection risk from Mycobacterium chimaera. This 2016 alert did not discuss any other heater-cooler models or bacteria as posing a risk.
(Article continues below)
Dr. Muscarella — Senior Technical Advisor: Dr. Muscarella provides expert opinions, case reviews and advice for consumers (and legal counsel), hospitals and device manufacturers about the causes of healthcare-associated infections (“HAIs”). Contact him (using your smart phone): Telephone | Email | Text (SMS) | Skype
(Article continues from above)
Notably, the CDC’s updated 2016 alert advises that hospitals “notify patients who underwent open-heart (open-chest) surgery involving a Stöckert 3T heater-cooler that the device was potentially contaminated, possibly putting patients at risk for a life threatening infection.” However, no federal law requires compliance with this CDC recommendation.
Informing the public of the possible cause of recent M. chimaera infections including one disclosed last year by the University of Iowa Hospitals and Clinics, the FDA’s Oct. 2016 alert reported that the Stöckert 3T model might have been contaminated with the NTM during manufacturing at the company’s facility, in Germany.
This FDA alert added that LivaNova had begun implementing cleaning and disinfection measures in Sept. 2014 to prevent this contamination.
Like the FDA’s Oct. 2016 alert, the CDC’s updated notice issued the same month also narrowed its focus (compared to its alert published a year earlier), now also singling out the Sorin 3T model and M. chimaera as posing the infection concern.
This CDC alert also now focused on a single cause, stating that “new information indicates that these devices, manufactured by LivaNova PLC, were likely contaminated with the rare bacteria M. chimaera during manufacturing” (overseas in Germany). The alert did not discuss any other possible causes, model of heater-cooler device, or NTM type that might pose a similar infection risk.
Quality, Safety and Case Reviews: Click here to read about Dr. Muscarella’s quality and safety services design to help hospitals, manufacturers and the public reduce the risk of healthcare-associated infections, including mycobacterial outbreaks linked to contaminated heater-cooler devices.
Update (March 9, 2017): In some cases — for example, in Los Angeles County — at least one hospital has linked a M. chimaera outbreak to a heater-cooler device, The Los Angeles Times has reported.
To date, however, health officials have not warned “at risk” patients of their potential exposure to the mycobacteria, or the specific symptoms that might indicate infection and warrant immediate medical attention.
In fact, although acknowledging the outbreak in February, county health officials have declined to name the hospital where this outbreak occurred, The Los Angeles Times has also reported.
The timely diagnosis and treatment of M. chimaera infections, as well as “close collaboration between device manufacturers and regulatory agencies to ensure safe use of the (heater-cooler devices), are essential to close this patient safety loophole,” two researchers have emphasized.
Scope too narrow?
Some researchers and organizations argue, however, that the FDA and CDC’s updated Oct. 2016 safety alerts may be too narrow in scope, primarily because neither advises the public that these types of infections have also been linked to (but not necessarily caused by) heater-cooler models sold by other manufacturers.
Nor does either updated alert advise the public that infections linked to contaminated heater-cooler devices have also been caused by bacteria other than M. chimaera.
According to a Nashville-based clinical services company that says it’s the largest provider of perfusion services in the U.S., the designs of all heater cooler models — not just the Sorin 3T’s — may be prone to bacterial contamination.
Seemingly agreeing, a cardiothoracic surgeon at St. Luke’s Hospital in Kansas City (MO) recently told a medical news source that, “the design(s) of all heater-cooler devices are inherently flawed [in that they] allow potential contamination and biofilm formation with dissemination to the patient via aerosolization from internal fans.”
Update (Feb. 9, 2017): Mycobacterial outbreaks linked to a contaminated heater-cooler devices have been identified in the U.S. and Europe — and now in other countries, too, including Canada, Australia and New Zealand.
Researchers in Australia now report that bacteria grown from an open-chest surgery patient’s bone marrow was identical to bacteria found in the heater-cooler device used at the time of surgery.
These Australian researchers also report that this patient’s M. chimaera genome closely matches that of bacteria that has infected patients in other parts of the world, suggesting the bacteria originated from a “point source,” as both the FDA and CDC had previously indicated.
Six heater-cooler device manufacturers
LivaNova, formerly the Sorin Group, is the manufacturer of the Stockert (or Sorin) 3T model, which is used by U.S. hospitals to perform cardiopulmonary bypass more than any other heater-cooler model. The price of these devices, purchased new, can be $35,000, or higher.
Approximately 60% of heart bypass procedures performed in the U.S. use the Sorin 3T heater-cooler device, according to the CDC.
 CardioQuip LLC (Bryan, TX), Cincinnati Sub Zero Products Inc. (Cincinnati, OH), Maquet Cardiovascular (Wayne, NJ), Medtronic (Mounds View, MN) and Terumo Cardiovascular Systems Corp. (Ann Arbor, MI) are the other five manufacturers who sell competing models in the U.S.
CardioQuip LLC (Bryan, TX), Cincinnati Sub Zero Products Inc. (Cincinnati, OH), Maquet Cardiovascular (Wayne, NJ), Medtronic (Mounds View, MN) and Terumo Cardiovascular Systems Corp. (Ann Arbor, MI) are the other five manufacturers who sell competing models in the U.S.
These less frequently used heater-cooler models include: the MCH-1000, the Hemotherm 400CE Heater-Cooler, the HCU 40 Heater-Cooler, the Bio-Cal 370 Blood Temperature Control Module, and the Terumo HX2 Temperature Management System, respectively.
M. chimaera is a slow-growing type of NTM. Certain other types of NTM like M. abscessus are fast-growing, however.
Infections of this latter type may therefore be diagnosed quickly and within days or weeks (and sometime a few months) after exposure, whereas those caused by M. chimaera may not be diagnosed until several years later.
That’s why health officials have concluded that patients who underwent open-chest surgery using a heater-cooler device as far back as 2011 may still be at risk of a M. chimaera infection.
Whether of the fast or slow-growing type, NTM are not ordinarily transmitted from one patient to another. Yet, they are “opportunistic,” generally causing infections only in patients who are already ill or have compromised immune systems.
Infections caused by NTM are usually treatable, although patients may not know they have been infected. Symptoms of infection include fever, pain, redness, and pus around the surgical incision.
Contaminated aerosols
Heater-cooler devices control the patient’s temperature by circulating heated and cooled water within a “closed loop” of tubes. This circulating water does not ordinarily directly contact the patient during surgery (although LivaNova has reported that contaminated water leaking from the heater-cooler device may also pose an infection risk).
Newly published data, however, suggest that a contaminated heater-cooler device can still pose a risk of infecting patients, albeit through indirect contact.
The FDA wrote in both its 2015 and updated 2016 alerts that although the water in the circuits does not come into direct contact with the patient, there is the potential for contaminated water to enter other parts of the device and aerosolize, transmitting bacteria through the air and through the device’s exhaust vent into the environment and to the patient.
In June 2016, researchers independently corroborated the FDA’s concerns, performing tests that confirmed contaminated heater-cooler devices can emit aerosols of M. chimaera into the operating room’s air, which could enter the patient’s open chest causing infection.
According to the FDA’s executive summary prepared for its advisory panel meeting the same month, “all (heater-cooler devices) have design features that could lead to aerosol formation.”
To reduce this risk, the FDA now advises hospitals to redirect the heater-cooler device’s exhaust vent away from the patient (or, either isolate the device in an enclosure or remove the device from the operating room).
If I was having cardiac surgery, I would want that machine out of the room. — Michael Edmond, an epidemiologist at the University of Iowa Hospitals & Clinics.
Recall of the Sorin (Stöckert) 3T Heater-Cooler
LivaNova has published that it first became aware of the risk of the Stockert 3T heater-cooler model emitting airborne mycobacteria three years ago, in January 2014.
Almost a year and a half later, in June 2015, LivaNova issued a field safety notice alerting users to the possibility that the Sorin 3T could become colonized with bacteria, and then aerosolize the bacteria into the operating room’s air, posing an infection risk.
The next month the company issued a voluntary recall of this model to further ensure users were aware that the device could become contaminated with mycobacteria “if proper disinfection and maintenance is not performed per instructions for use.”
This recall did not require that the 3T model be removed from U.S. hospitals, however, only that hospitals be more vigilant about this device’s decontamination instructions and requirements.
Three months later, on Oct. 15, the FDA issued the first of its two aforementioned alerts warning that heater-cooler devices used in the U.S. could pose a risk of transmitting NTM, via the air, into the open-chest cavity of surgery patients.
By the end of 2015, the FDA had increased its oversight of these devices, warning LivaNova in a Dec. 29 letter that the Sorin 3T model was both “adulterated” and “misbranded.” The letter further advised the company that this model requires a new legal clearance or regulatory approval, in part to assure that “appropriate testing and validation of the cleaning/disinfecting protocols have taken place.”
The FDA’s 2015 warning letter also advised LivaNova that these devices “are subject to refusal of admission” into the U.S.
This is a manufacturer problem. … All machines can emit aerosol. (The risk of a heater-cooler device transmitting aerosolized bacteria into the air and sterile field) is not (a) 3T-specific problem. … we have been able to measure aerosolization from, emitted from all (the manufacturers’) devices. — A LivaNova representative (during the FDA’s June 2-3, 2016 panel meeting).
Other models are prone to contamination, too
Investigations, like that of a South Carolina M. abscessus outbreak in 2014, had initially linked only the Sorin 3T model to mycobacterial infections in open-chest surgery patients.
But other heater-cooler models, too, may be similarly prone to bacterial contamination, according to SpecialtyCare, the Nashville-based clinical services company.
In June SpecialtyCare issued a clinical alert that stated, in part: “Due to design characteristics, all (heater-cooler devices), regardless of manufacturer, are susceptible to” the development of bacterial biofilms on some of their surfaces.
This clinical alert added that, “The rate of reported incidents among different machine types is proportionate to the volume of market share of each manufacturer, and changing devices may not alleviate the problem. No device has been found to be less susceptible to biofilm deposition than another.”
Notwithstanding its Oct. 2016 updated alert focusing on the Sorin 3T model, the FDA has previously advised that “the designs of most heater-cooler devices are similar” (e.g., featuring vents, fans and water tanks).
Also according to the FDA, “all of the heater-cooler devices in distribution have design aspects that agitate the water and have fans with the potential to disrupt the laminar air flow in operating rooms.” The FDA further adds that these fans “may facilitate the movement of aerosolized (mycobacteria) from the inside of the (heater-cooler device) into the operating room, and possibly into the sterile surgical field.”
Moreover, in the executive summary that the FDA prepared for an advisory panel meeting the agency hosted last June to discuss the risk of heater-cooler devices infecting patients, the FDA wrote that “all (heater-cooler devices) have design features that could lead to aerosol formation.”
After talking with consumer advocates and health experts including those at the CDC about other heater-cooler device brands, not just the Sorin 3T, being prone to mycobacterial contamination, The Washington Post wrote that “these machines operate in similar ways. They could be contaminated in similar ways and also pose infection risk.”
And, Consumer Reports reported in November that, “So far, the vast majority of (identified infection clusters) have involved … (LivaNova’s) Stöckert 3T.” But it added that “at least three other companies’ devices have also been linked to bacterial contamination worldwide, and both the FDA and CDC have acknowledged that the concern goes beyond any one brand.”
While acknowledging that the CDC’s advisory last October recommended hospitals notify patients who underwent open-heart surgery using the Sorin 3T heater-cooler of this infection risk, Consumer Reports points out that the CDC’s advice may not “go far enough, in part because it should extend to all hospitals using any brand of heater-cooler” — not just the Sorin 3T.
LivaNova would seem to agree, writing its customers in Oct. 2015 that, “Our investigation has shown that contamination by mycobacteria is a general problem affecting all heater-coolers used in the operating room and is not restricted to Sorin heater-coolers. This has been further confirmed by a recent communication issued by the FDA in October 2015.”
Quality, Safety and Case Reviews: Click here to read about Dr. Muscarella’s quality and safety services design to help hospitals, manufacturers and the public reduce the risk of healthcare-associated infections, including mycobacterial outbreaks linked to contaminated heater-cooler devices.
 Another heater-cooler device is found to be contaminated with an outbreak’s Legionella bacteria
Another heater-cooler device is found to be contaminated with an outbreak’s Legionella bacteria
Bacterial infections in open-chest surgery patients have been recently linked to the use of models other than the Sorin 3T heater-cooler device, too.
CardioQuip, LLP (Bryan, TX) manufactures the Modular Cooler Heater (MCH) 1000 series, which are two heater-cooler models designed to reduce the risk of bacterial colonization on its internal surfaces and water reservoir, according to the manufacturer.
In September, while investigating the cause of a deadly Legionella outbreak, a Seattle (WA) hospital found a number of CardioQuip heater-cooler devices to be contaminated with the bacteria, according to The Seattle Times.
Legionella bacteria cause Legionnaires’ disease, a potentially deadly respiratory infection.
Confirming the outbreak, the University of Washington Medical Center released a letter on Sept. 20 announcing that four patients have been diagnosed with Legionella pneumonia, two of whom died. While Legionella bacteria may have been a contributing factor, an official cause of death has not been determined, a hospital executive wrote in the letter.
Heater-cooler devices store water in internal tanks. Hospitals may sometimes fill these tanks with tap water, although the FDA recommends that only sterile or filtered water be used. Ice may also be used during these open-chest surgery procedure to cool the heart.
Unlike sterile water, tap water can contain Legionella, although infrequently and usually in numbers too low to harm the public.
UWMC identified Legionella in some of the hospital’s water, The Seattle Times also reported.
In addition to the heater-cooler device and some of its tap water, UWMC found an ice machine and two sinks to be contaminated with the Legionella bacteria. As with heater-cooler devices, the FDA recommends that sterile or filtered water be used to make ice used during open-chest surgeries.
Although the Legionella was found in the hospital’s heater-cooler devices, UWMC told The Seattle Times it suspects the outbreak was more likely due to the patients’ exposure to the hospital’s tap water, possibly the contaminated ice machine or sinks.
Update (June 11, 2024): Seidelman et al. (2024) reported a clonal cluster of three extrapulmonary M. abscessus infections among patients who had undergone cardiothoracic surgery at a hospital in North Carolina. An investigation linked this cluster to M. abscessus contamination of a water-based CardioQuip heater-cooler model. The clone responsible for this cluster of infections “most likely originated from the municipal water supply” (i.e., the hospital tap water), these authors wrote.
Using a different heater-cooler model (the Stöckert 3T) to perform cardiopulmonary bypass surgery at the same North Carolina hospital, Baker et al. (2017), whose authors included several contributors to the Seidelman et al. (2024) paper, had epidemiologically linked a different 2-phase clonal outbreak of M. abscessus seven years earlier to colonized hospital tap water.
Acknowledging that NTM are often present in hospital water, Baker et al. (2017) reported several primary interventions to reduce the risk of infection including water engineering changes designed to decrease NTM burden in the hospital’s plumbing system.
Note: For clarification, bacterial contamination of a reusable medical device is not, by itself, sufficient for infection. To cause an infection, the heater-cooler device would have to expose the patients to the bacteria — for example, via contaminated aerosols that could enter the patient’s open-chest cavity. When used outside of the operating room, heater-cooler devices would not be expected to pose an infection risk even if contaminated with NTM.
Maquet’s urgent safety notice: A timeline
Not only LivaNova, but other companies selling these devices in the U.S. have also notified hospitals about the risk of infection associated with contaminated heater-cooler devices.
A month after the FDA and CDC began notifying healthcare providers about the potential for heater-cooler devices to transmit deadly infections, Maquet issued an urgent notice called a “field safety corrective action,” or FSCA, on Nov. 30, 2015.
This notice stated that the company has “confirmed that Maquet systems used (during cardiac bypass surgery) are contaminated with various strains of bacteria that also include Mycobacteria species.”
Acknowledging that four of its heater-cooler models could become contaminated with mycobacteria, Maquet’s notice provided an updated procedure for decontaminating these models, which include the Maquet HCU 30 and 40 models.
This updated procedure is necessary, according to this notice, because Maquet has “confirmed that the current published cleaning and or decontamination procedures (in the Instructions for Use) is not sufficient and may not completely remove (biofilms) that may accumulate over time in contaminated systems.”
Three months earlier in Aug., Maquet had filed a regulatory report with the FDA stating that, “a new (field safety corrective action) will be issued as soon as the new disinfection procedure is properly validated and can be launched. The new (instructions for use) is currently under revision and will contain the instructions for the new disinfection procedure.”
On Dec. 10, two weeks after issuing the first notice, Maquet issued a second field safety corrective action, or FSCA, informing users that the Nov. 30th FSCA had been put “on hold.” Users were advised to revert back to using the device’s original decontamination procedure.
According to this Dec. 10th notice, the revised decontamination procedure (apparently like the original procedure provided in the device’s manual) had not been sufficiently validated.
Also in the late fall of 2015, Maquet recalled its HCU 30 heater-cooler model used in the U.S., but this action do not appear related to an NTM infection.
Three months later, on March 11, 2016, Maquet filed another regulatory report with the FDA stating (at least for European users of the Maquet HCU 40 model) that “a new (safety alert) will be issued as soon as the new disinfection procedure is properly validated and can be launched” — adding that “December 2016 is the scheduled market launch of this new disinfection procedure.”
Then, in Sept. 2016, Maquet issued a worldwide recall of the HCU 30 model alerting customers of “the potential for contaminated water to enter parts of the Heater-Cooler Unit circuits. There is the potential risk of bacterial contamination including Mycobacteria species.”
Update: In April 2017, Maquet informed the FDA that a hospital had cultured mycobacteria from the water in a Maquet HCU 40 device. The report concludes that no patients were infected.
According to the regulatory report Maquet filed, the company is developing new decontamination protocols for the HCU 40 (and 20 and 30) heater-cooler device. This report added that the timeline for the release of these new protocols are “being examined in order to communicate reliable dates as requested by health authorities.”
While these notices, Sept. recall, and regulatory reports suggest Maquet’s heater-cooler devices are prone to bacterial contamination, I did not identify any adverse event reports filed with the FDA linking a Maquet heater-cooler device directly to a bacterial infection.
We’ve only begun to scratch the surface, even though it has been going on for 2 years. … The incidence (of infections linked to heater-cooler devices) is likely underreported. — Keith Allen, MD (St. Luke’s Hospital in Kansas City, MO)
Update (March 2017): A March 2017 study by Svensson et al. (2017) found that four of five (80%) Maquet heater-cooler devices (used in Denmark) were contaminated with M. chimaera.
Their study concludes not only that heater-cooler devices other than the Sorin 3T model are prone to mycobacterial contamination, but also that “mycobacterial contamination might be a general problem for (all heater-cooler devices).”
These findings are somewhat at odds with the FDA and CDC’s conclusion, however, which in Oct. 2016 reported that only patients on whom the Sorin 3T model (not the Maquet or another manufacturer’s heater-cooler device, Svensson et al.’s later findings notwithstanding) was used during open-chest surgery are at risk of these life-threatening mycobacterial infections.
MedPage Today reports that “While the LivaNova/Sorin 3T heater-cooler device for heart surgery has gotten the lion’s share of attention over Mycobacterium chimaera infections, every similar device on the market has contamination reported and most have infected patients.”
Heater-cooler devices sold by all five of the manufacturers have been linked to contamination in the FDA’s adverse-event database, and four of the five manufacturers’ devices have been linked to patient infections; three have been linked to patient deaths, according to this MedPage Today article. (Note: I identified six, not five, heater-cooler manufacturers; see above.)
![]() Connecting the dots: Click here to read about Dr. Muscarella’s quality and safety services designed to reduce the risk of healthcare-associated infections. These services include his searching multiple databases to identify otherwise undisclosed adverse events linked to medical devices.
Connecting the dots: Click here to read about Dr. Muscarella’s quality and safety services designed to reduce the risk of healthcare-associated infections. These services include his searching multiple databases to identify otherwise undisclosed adverse events linked to medical devices.
Medtronic’s heater-cooler is linked to an NTM infection
The FDA was notified three times last year that the Medtronic Bio-Cal 370 Blood Temperature Control Module had been linked to bacterial infection.
Medtronic filed a regulatory report in Oct. 2015 informing the FDA that this model had been linked to a M. abscessus infection — the same NTM type responsible for the South Carolina hospital’s mycobacterial outbreak linked to the Sorin 3T a year earlier — approximately 5 months after a patient underwent aortic valve replacement surgery. (Remember that M. abscessus is a fast-growing NTM, whereas M. chimaera is a slow growing NTM.)
The hospital initially removed the Medtronic device from use, but then returned it to service after “sterilizing” it, according to the regulatory report, which appears to be Medtronic’s response to a separate regulatory report a hospital filed a month earlier, on Sept. 24th, that contains similar details.
A third regulatory report that a hospital filed two weeks earlier on Sept. 11th informed the FDA of the Bio-Cal 370’s association with a patient death. The report provides no other details.
Despite these three regulatory reports, none of the FDA’s safety communications, meeting notes, or health alerts warning the public about the infection risks that a contaminated heater-cooler device might pose includes the Medtronic Bio-Cal 370 as a device that had been linked to infections following open-heart surgery.
In fact, while discussing each of the other heater-cooler models sold in the U.S., the FDA’s executive summary prepared for the circulatory advisory panel meeting it hosted last June does not include the Bio-Cal 370 model (refer to this FDA executive summary’s Tables 1, 2, 4 and 5). (The reasons for this apparent omission are unclear.)
Moreover, the FDA and CDC’s updated alerts from last October focus on M. chimaera, without recognizing M. abscessus — the strain discussed in two of these regulatory reports involving the Bio-Cal 370 (as well as being linked to the deadly outbreak in South Carolina in 2014) — as a type of mycobacteria that could also infect patients during open-chest surgery on cardiopulmonary bypass.
Cincinnati Sub Zero issues a press release
In the wake of the FDA’s Oct. 2015 alert to healthcare providers, other companies that sell heater-cooler devices in the U.S. also notified hospitals about the importance of using an effective decontamination procedure to prevent infections.
On Nov. 12, 2015, Cincinnati Sub Zero issued a press release recommending that users strictly follow the decontamination procedures described in the heater-cooler device’s operator’s manual “to minimize the risk of bacterial growth and subsequent patient infection.”
In Oct. 2011, almost four years earlier, the company had recalled a Hemotherm model (the specific model is not named in the recall notice) because the device had not been cleared by the FDA prior to distribution.
The next year on Dec. 18, 2012, the FDA cleared the company’s Hemotherm 400CE Heater-Cooler model. Likely in response to this clearance, the FDA “terminated” this recall two months later. (This device’s predicate, the Hemotherm 400, was cleared in 1981.)
The FDA has received a few reports of bacteria being cultured inside the Hemotherm device, but I did not identify any reports in the agency’s medical device database linking a Cincinnati Sub Zero heater-cooler devices to a bacterial infection in an open-heart surgery patient.
Terumo enters into consent decree with FDA in 2011
Heater-cooler models sold by Terumo, a sixth manufacturer of these devices, have also been censured.
Five years ago, the sale of Terumo’s heater-cooler devices had been stopped when the company entered into a consent decree with the FDA.
In March 2011, the FDA issued a statement entitled, “FDA: Michigan heart-lung bypass machine manufacturer enters into consent decree.” One of this consent decree’s terms required Terumo to pay a fine of $35 million.
This consent decree also prevented Terumo from manufacturing and distributing to new customers several different cardiovascular devices, including the HX2 Temperature Management System and the Sarns TCM II Cooling and Heating System, which are heater-cooler devices.
The FDA would permit Terumo to sell these devices to current customers, but only once the company had demonstrated it had become compliant with the FDA’s requirements overseeing good manufacturing practices and medical device reporting.
[The Terumo HX2 heater-cooler model, which the FDA cleared in 2007, is an updated version of the technologies from two of the company’s other heater-cooler devices: the Sarns TCM II and the Sarns Dual Heater-Cooler, according to the manufacturer. The FDA cleared the Terumo TCM II model in 1988, but the Sarns Dual Heater-Cooler device is a “pre-amendment” device that, using a legal loophole, does not require a pre-market clearance, according to Terumo.]
According to the FDA’s statement, Terumo entered into this consent decree with the FDA in 2011 because inspections of its facility in Ann Arbor (MI) the previous year revealed numerous regulatory violations that raised safety concerns, including deficiencies in its procedures for controlling the design of its devices, including the HX2 heater-cooler device.
According to the Ann Arbor News, four FDA investigators who inspected the company in 2010 concluded that Terumo had “not implemented an adequate and effective quality system at all levels of your organization.”
Years earlier, the FDA had censured Terumo for violating certain regulatory standards, issuing warning letters to the company in 2004 and 2006. In Feb. 2015, Terumo recalled the HX2 model (but this action appears unrelated to mycobacterial infections).
Last June Terumo issued another recall, this time to notify users that the disinfectant, or sanitizer, described in the cleaning instructions of third model, the Sarns Dual Heater-Cooler, was no longer available.
Terumo’s consent decree lifted just months ago
Also in June of 2016, Terumo reported that the FDA had lifted the 2011 consent decree.
According to the company, the FDA had informed it two days earlier that: “Terumo is no longer enjoined under Paragraph 5 of the consent decree from manufacturing, packing, storing, installing, and/or distributing” the several devices the FDA censured in 2011, including the HX2 heater-cooler model.
This manufacturer’s press release stated, too, that the FDA had inspected its Ann Arbor (MI) facility in May 2016 and found “no inspectional observations.”
Yet, beginning in late Dec. 2015 — six months prior to lifting this consent decree — Terumo notified the FDA four times that a hospital had linked the company’s HX2 heater-cooler model to four M. abscessus infections and two deaths, my research has found.
I discuss these M. abscessus infections in a related article I wrote entitled, “A Less Commonly Used Heater-Cooler Device Also Linked To Mycobacterial Infections.”
Last spring, a hospital reported that another heater-cooler model sold by Terumo — the Sarns TCM-II — had tested positive for M. chimaera contamination. According to the regulatory report Terumo filed with the FDA, no patients were infected.
Whether the FDA had confirmed that Terumo had validated the effectiveness of its heater-cooler devices’ respective decontamination instructions prior to lifting the consent decree in June, as Terumo has reported, allowing the company to begin reselling heater-cooler models is unclear.
Data validation
In general, FDA requires that the decontamination procedures of reusable medical devices — including heater-cooler devices — be validated prior to selling the device to U.S. hospitals, in part, to ensure the device’s effectiveness and to reduce the likelihood of patient infections.
In December of 2015, the Pennsylvania Department of Health (PA-DOH) published a health advisory, however, acknowledging that it does “not currently have data to validate or refute the efficacy of (heater-cooler unit) manufacturers’ disinfection procedures to prevent (mycobacterial) contamination, colonization and transmission.”
This PA-DOH’s conclusion appears to raise questions about the current regulatory status of heater-cooler devices.
“Nobody has found a way to be able to decontaminate these (heater-cooler) machines to an extent that it would actually be able to rid the machines 100% of all bacteria.” — The Director of Quality Resources for a New York hospital.
The PA-DOH’s advisory expressed more concern, writing that, “it is unknown whether risk of (mycobacterial) infection can be completely eliminated given the paucity of data with which to validate device engineering and manufacturers’ most recent (instructions for use).”
This assessment is consistent with research published in Oct., which found that, “despite an intensified cleaning and disinfection protocol,” heater-cooler devices that were tested remained contaminated with mycobacteria.
More from Consumer Reports
Consumer Reports advised hospitals last November to notify all patients who have been exposed to any heater-cooler model since 2011 about this infection risk.
Consumer Reports is a nonprofit organization dedicated to unbiased research and education. As described on its website, Consumer Reports’ primary mission is to provide consumers “with the trusted knowledge they depend on to make better, more informed choices.”
Published since 1936, this American magazine has approximately 4 million print subscribers and 3 million on-line (digital) subscribers, the Atlantic magazine reported in April.
More than 250,000 heart bypass procedures using heater-cooler devices are performed in the U.S. every year using heater-cooler devices sold by LivaNova and its competitors. Worldwide, more than one million cardiac operations are performed annually using a heater-cooler device.
At least in the U.S., therefore, if hospitals follow the CDC’s recommendation, approximately 750,000 “at risk” patients (who underwent surgery since 2011) would be notified in the coming weeks of their potential exposure to life-threatening bacteria during their surgical procedure.
More than one million “at risk” patients likely would be notified if U.S. hospitals were to adopt Consumer Reports’ advice and notify all patients who underwent open-heart (open-chest) surgery since 2011 using any heater-cooler device (not just the Sorin 3T model).
Tap water, ice: sources of NTM contamination?
Unlike its safety alert published the previous year discussing the risk of heater-cooler devices infecting patients with mycobacteria, the FDA’s updated Oct. 2016 alert singled-out, by name, the Sorin 3T model as posing the concern.
This 2016 federal alert also emphasized that some Sorin 3T models may have been contaminated with mycobacteria during manufacturing in Germany, posing an infection risk here in the U.S.
But published data suggest that more than one factor — not just a manufacturing misstep — may have contributed to some of these recent bacterial outbreaks confirmed in the U.S.
For example, tap water, which (at least in the past) may be used to fill the heater-cooler device’s reservoirs, not only can be contaminated but has been linked to some mycobacterial outbreaks, suggesting that intrinsic contamination of the Sorin 3T heater-cooler device with NTM during manufacturing may not be the sole cause of these outbreaks.
Indeed, notwithstanding the FDA’s alert the previous month (like the CDC’s Oct. 2016 advisory, too) focusing solely on a different cause of the nation’s recent spate of mycobacteria outbreaks: contamination of the 3T heater-cooler during the device’s manufacturing in Germany, the FDA informed hospitals in Nov. of the following: “Be aware that device contamination also may occur from other sources such as environmental contamination …”
An example would be tap water. (Remember, as discussed above, that UWMC has concluded that patient exposure to contaminated tap water was the likely cause of its Legionella outbreak last year that affected open-chest surgery patients.)
As I discuss in more detail in a related article I wrote, the four regulatory reports Terumo filed with the FDA cite contaminated tap water as being a possible cause of mycobacterial infections recently linked to a heater-cooler device.
And, although not often discussed, ice used during open-chest surgeries, especially if produced from tap water (or inadequately filtered water), can be a source of NTM infections.
Used along with a heater-cooler device, ice may be used during open-chest surgeries to cool the heart. If the ice is contaminated with mycobacteria, however, its use in the surgical field could pose a serious infection risk.
Appreciating this potentially under-emphasized risk, the FDA recommended in Oct. that, “when making ice needed for patient cooling during surgical procedures, use only sterile water or water that has been passed through a filter of less than or equal to 0.22 microns.”
An on-line source (HeartValveSurgery.com) provides a picture of an open-chest surgical procedure reputedly displaying ice chips on the heart’s tissue.
Consumer Reports noted in Nov. that some hospitals may use an older, “less efficient” heater-cooler model that requires “the use of additional non-sterile equipment, including ice machines, which can introduce additional contamination risks.”
According to the FDA, “water filters (0.2 micron) should be able to remove most NTM from tap water that is used in filling/refilling, topping off, rinsing, making ice and cleaning the heater cooler units.”
How a hospital would be alerted and know when the filter is no longer working properly is unclear. A water filter’s use-life depends on several not-easily-identifiable factors, including the microbial quality of the water.
In June, LivaNova recalled the Stockert 3T’s ice container in Canada “to further mitigate the potential risk of infection by (NTM).” According to the company, the container “could be a source of contamination of the heater-cooler 3T’s water circuit if the user has failed to follow the instructions for use for water maintenance and water circuit disinfection.”
The risk of NTM infections posed by contaminated ice, as much or more so than contaminated tap water, a hospital’s unwitting use of an ineffective water filter, or contamination of the heater-cooler device during manufacturing, is unclear.
Mycobacterium abscessus also a risk
Bacterial outbreaks linked to contaminated heater-cooler devices are not limited to the Sorin 3T model — or to M. chimaera.
For example, M. abscessus, not M. chimaera, was the cause of the South Carolina hospital’s outbreak in 2014.
M. abscessus was also the organism identified by Terumo in the four regulatory reports that the company filed with the FDA in Dec. 2015 and Jan. 2016. I discuss these regulatory report in more detail in my related article entitled, “A Less Commonly Used Heater-Cooler Device Also Linked To Mycobacterial Infections.“
And, M. abscessus is named in the regulatory report Medtronic filed with the FDA as the bacteria that caused the infection in Oct. 2015.
In fact, LivaNova’s June 2015 field safety notice warned users that the water in heater-cooler devices can be contaminated with other waterborne pathogens, too, including M. abscessus.
These reports linking heater-cooler devices to M. abscessus outbreaks suggest that tap water can also be a source of NTM infections in open-chest surgery patients.
Update (March 2017): Baker et al. (2017) investigated and mitigated a two-phase clonal outbreak of M. abscessus linked to hospital tap water.
Twelve (50%) of 24 “phase 2” cases occurred in cardiac surgery patients with invasive infections. This phase was resolved after the investigators implemented an intensified disinfection protocol, in addition to using sterile water in the heater–cooler devices.
Contaminated duodenoscopes: Deja vu?
In 2015, similar concerns were voiced that federal health officials were slow to warn the public about the risk of another device — contaminated duodenoscopes — unwittingly transmitting deadly superbug infections to unwarned patients.
Sen. Patty Murray (D-WA) published an investigative report earlier this year that concluded, among other findings: “While FDA started investigating how closed-channel duodenoscopes cleaned according to manufacturers’ instructions spread infection in September of 2013, the agency took no action to alert hospitals, doctors and the public to the risk posed by closed-channel duodenoscopes for 17 months.”
The Senator’s report added that, “At least 68 patients in seven different hospitals in the United States were infected with antibiotic-resistant bacteria linked to duodenoscopes during this period.”
Summary and closing remarks
A few final remarks: First, infections in open-chest surgery patients have been linked to the use of heater-cooler devices other than the Stockert 3T.
Second, in addition to slow-growing M. chimaera, fast-growing M. abscessus has been linked to infections in patients who underwent open-chest surgery using a heater-cooler device. Regulatory reports discussed in this article link use of three different heater-cooler models during open-chest surgery to M. abscessus infections.
Third, the incidence of heater-cooler devices infecting patients with mycobacteria and other types of bacteria may be significantly higher than public health officials have publicly recognized.
Fourth, a South Carolina hospital’s NTM outbreak in June 2014 was the first publicly reported in the U.S. to be linked to a contaminated heater-cooler device.
Fifth, both heater-cooler devices and duodenoscopes reveal significant gaps in the federal oversight of medical devices.
Sixth, Consumer Reports recommends that hospitals notify all patients who underwent open-chest surgery using a heater-cooler device since 2011 about the risk of a life-threatening mycobacterial infection.
Last, the rationale for federal warnings and advisories in 2016, compared to those issued in 2015, to narrow the focus, reduce the scope of the risk, and warn that only one heater-cooler model (the Sorin 3T) is prone to contamination with one type of mycobacteria (M. chimaera) due to one particular cause (a flawed manufacturing process overseas) is not obvious.
The facts suggest a different conclusion: that the infection risk may be broader in scope and higher than publicly acknowledged, and that certain other heater-cooler models, in addition to the Sorin 3T, are prone to contamination and not just with M. chimaera, but also with M. abscessus (and possibly other types of microorganisms), due to at least one other possible cause: contaminated tap water (and/or ice).
Update (Sept. 30, 2020): Consistent with the findings of this article published in 2017, the FDA issued a letter almost three-and-a-half years later to healthcare providers focusing on the potential risk of infection during cardiac surgery when using the CardioQuip Modular Cooler-Heater Device. The letter concluded that based on learning about a new cluster of infections associated with this model, FDA acknowledges that it is “now aware of NTM patient infections, NTM device contamination, or both issues, for all the manufacturers of heater-cooler devices in the United States.”
This FDA letter, issued on September 30, 2020, therefore cautioned “health care providers and users to be aware of and remain vigilant for the potential risk of NTM infections in patients who have undergone cardiothoracic surgeries using any heater-cooler device.”
Five months after issuing this Sept. alert, FDA received a report filed by a user facility linking this CardioQuip MCH device to a patient who developed Serratia bacteremia/sepsis after cardiac and renal transplantation, and who later expired. According to the facility’s account, “the tubing inside the machine had extensive buildup of biofilm. While it is unknown whether this contributed to the infection, it was very concerning.” The report does not discuss whether the biofilm included Serratia.
Not unlike concerns the FDA published beginning in 2015 about the ineffective reprocessing of another type of reusable device called a duodenoscope, this facility’s 2021 report (discussing this HCD model) states that “[i]t appears that once the biofilm gets established, the cleaning/ disinfection process in the (HCD’s instructions for use) is not adequate to remove it.” The facility adds in the report that it “contacted the manufacturer about the biofilm, but they were unable to suggest a way to remediate the problem and do not have loaner machines available.”
The report notes that the device’s instructions for use do not state “how to mitigate extensive buildup. The preventive maintenance instructions in the manual do not include checking for biofilm buildup on the interior pump tubing.” To prevent transmission of diseases, the safe design of virtually every reusable medical device, including duodenoscopes and HCDs, requires, in part, that its reprocessing (and maintenance) instructions be validated for effectiveness and completeness.
Note: Regulatory reports submitted to the FDA by a manufacturer or user facility can describe important clinical cases and experiences associated with a medical device’s use. However, the findings and conclusions of these reports generally have not been independently reviewed, and therefore may be incomplete and/or inaccurate.
Article by: Lawrence F Muscarella, PhD. Posted: January 11, 2017. LFM Healthcare Solutions, LLC Copyright 2017. LFM Healthcare Solutions, LLC. All rights reserved.
Lawrence F Muscarella PhD is the owner of LFM Healthcare Solutions, LLC, a Pennsylvania-based quality improvement and consulting company that provides safety services for hospitals, manufacturers and the public. Email Dr. Muscarella for more details.