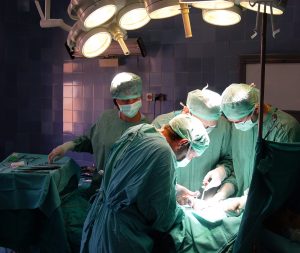
June 24, 2017 –– Gastrointestinal endoscopes used at a U.S. air base in the Middle East were incorrectly cleaned, possibly exposing patients to HIV and the hepatitis B and C viruses, the Air Force Surgeon General Public Affairs Office announced in a press release issued on Monday, June 19th.
 In response, the Air Force Medical Service has now begun notifying potentially infected patients of the risk. It is also providing medical counseling, and recommending that the patients receive diagnostic testing for bloodborne viral infections.
In response, the Air Force Medical Service has now begun notifying potentially infected patients of the risk. It is also providing medical counseling, and recommending that the patients receive diagnostic testing for bloodborne viral infections.
AFMS determined that as many as 135 patients at the Al Udeid Air Base in Qatar could have been infected with these viruses while undergoing upper and lower GI endoscopy, according to the June 19th press release.
The air base used these potentially contaminated endoscopes to perform these procedures during an eight-year period, between April 2008 and April 2016.
While the risk of infection during GI endoscopy is reported to be low, viral infections linked to GI endoscopy have been documented.
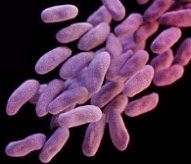
Deadly outbreaks caused by multidrug-resistant bacteria, including CRE and related “superbugs,” have similarly been linked to contaminated GI endoscopes. The mortality rate of such CRE infections can be as high as 50%.
Highlights:
- The failure by the Al Udeid Air Base in Qatar to properly clean and disinfect both upper and lower GI endoscopes began in 2008 posing an infection risk for as many as 135 patients, according to the Air Force.
- The Air Force has just begun notifying these potentially exposed patients – 14 months after the breach was reportedly identified and corrected.
- Less than a year after this air base’s reprocessing error began, three Veterans Affairs medical centers in 2009 notified close to 10,000 U.S. veterans of their potential exposure to bloodborne pathogens as a result of similarly using improperly sanitized endoscopic equipment.
- My perspective and opinions are provided.
- Recommendations to prevent the recurrence of this type of cleaning lapse are provided.
- 23 patients who underwent upper and lower GI endoscopy at a hospital in Largo (MD) were similarly notified last week of an infection risk linked to contaminated medical equipment. This incident is briefly discussed.
Although this Qatari air base’s failure to correctly reprocess these GI endoscopes consistent with sterilization safety standards was first identified last year in April 2016, according to Monday’s press release, the Air Force is only now warning patients of the potential infection risk — more than a year later.
Monday’s press release does not discuss the circumstances surrounding the Air Force’s discovery last year of this 8-year-long breach.
Factors typically responsible for a medical facility’s identification of such an infection-control breach include routine surveillance, the investigation of an infection caused by a concerning pathogen, a news report, a federal alert, or a staff member’s complaint about an unsafe practice.
[Article continues below]
Technical Advisor: Dr. Muscarella provides expert opinions, case reviews and advice for hospitals, device manufacturers and consumers about the causes of healthcare-associated infections (“HAIs”) linked to contaminated upper and lower GI endoscopes, among other devices. Contact him (using your smart phone): Email | Text (SMS) | Skype
[Article continues from above]
Medical technicians at this Qatari air base had been using “an alternate cleaning method” to reprocess GI endoscopes, instead of a recommended automated process, Monday’s press release further reports.
 A spokeswoman for the Office of the Air Force Surgeon General told Military.com (via an email) that “during equipment reprocessing, the flushing and brushing of the (endoscope’s channels) were not completed as recommended by the manufacturer.”
A spokeswoman for the Office of the Air Force Surgeon General told Military.com (via an email) that “during equipment reprocessing, the flushing and brushing of the (endoscope’s channels) were not completed as recommended by the manufacturer.”
More than 9,000 service members and civilians live and work at this air base, which is one of the largest U.S. military bases in the Middle East. It is located 20 miles southwest of the Qatari capital of Doha.
Brig. Gen. Robert Miller, the Air Force Medical Operations Agency commander, stated in Monday’s press release that, “Providing quality health care to our Airmen and their families is our top priority.”
For its part, the Air Force apologized to the affected patients, assuring them that, “appropriate actions have been taken to address and mitigate the causes that led to this problem.”
The preventive actions that the Air Force has since taken include a “service-wide patient safety alert” intended to prevent this breach’s recurrence by confirming that medical technicians responsible for reprocessing GI endoscopes are adhering to proper “endoscope cleaning, decontamination, inspection and sterilization processes.”
But the clinic’s actions and concern apparently are not limited to GI endoscopes.
Additionally, Air Force military treatment facility commanders have been directed to review the reprocessing practices of all reusable medical instruments, according to the Air Force’s June 19th press release. It is unclear whether this directive applies only to this Qatari air base, or to medical facilities associated with all the U.S. Armed Forces.
The Al Udeid Air Base clinic is no longer performing endoscopy or colonoscopy.
Quality, Safety and Case Reviews: Click here to read about Dr. Muscarella’s quality and safety services design to help hospitals, manufacturers and the public reduce the risk of healthcare-associated infections, including superbug outbreaks linked to contaminated reusable medical equipment.
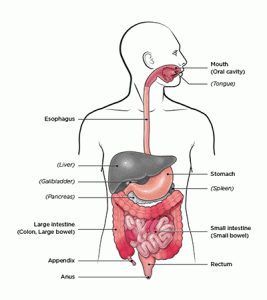
What is “upper” and “lower” GI endoscopy?
A gastroscope is the most well-known type of “upper” GI endoscope, so named because it is used in the upper GI tract. This endoscope type is used to perform esophagogastroduodenoscopy, or “EGD” – a procedure that examines and treats diseases of the lining of the esophagus, stomach, and first part of the small intestine, called the duodenum.
EGD may also be referred to more simply as “endoscopy.”
A duodenoscope is another type of upper GI endoscope. It is used to perform endoscopic retrograde cholangiopancreatography, or “ERCP” – a procedure that uses x-rays during upper GI endoscopy to diagnose and treat disorders of the bile and pancreatic ducts.

A colonoscope is the most common type of lower GI endoscope, so named because it is used in the lower GI tract. This endoscope type is used to perform colonoscopy – a procedure that examines diseases primarily of the colon.
My perspectives, opinions
Monday’s disclosure by the AFMS brings into acute focus the importance of correctly cleaning and disinfecting GI endoscopes and other reusable medical devices in compliance with the manufacturer’s instructions (and sterilization standards), lest patients be exposed to potentially life-threatening pathogens and then be warned of the potential infection risk.
But as well as revealing safety gaps, this AFMS press release, like this air base’s reprocessing breach, raises several questions.
Risk assessment performed? For instance, the AFMS determined that as many as 135 patients of this Qatari clinic may be at risk of contracting a bloodborne viral infection from a potentially contaminated upper or lower GI endoscope.
This assessment would indicate that the Al Udeid Air Base performs, on average, seventeen (17) GI endoscopic procedures at the clinic per year – or fewer than 2 procedures per month.
This number seems low. Although it certainly may be accurate, this calculation raises the question whether more GI endoscopic procedures may have been performed annually at the clinic since 2008, but that the AFMS deemed some patients not to be at risk for an infection, and therefore did not notify them of the breach. This possibility warrants further investigation.
“Timely” notification? Monday’s press release discloses that this Qatari clinic’s infection-control breach, which began in 2008, was not identified until eight years later, in April 2016 — more than a year ago.
These dates presumably indicate that the Air Force Medical Service has been aware of this potentially significant breach for as many as 14 months, but did not publicize it until a few days ago, on June 19th.
The rationale for delaying the notification of the air base’s GI endoscopy patients “at risk” for a bloodborne viral infection is unclear (and may suggest some initial confusion about this breach’s true infection risk).
Prompt notification of patients who may have been exposed to an endoscope contaminated with an infectious pathogen, especially a bloodborne pathogen, would seem necessary as a matter of proper protocol and disclosure, to prompt the patients to be tested for infection, and to prevent the disease’s unwitting transmission to others.
According to a study published in 2010 by researchers at the University of Washington School of Medicine, “from a purely utilitarian perspective, disclosure of large-scale adverse events is ethically appropriate even when the chance that any patients have been physically harmed is extremely low.”
These Washington researchers further wrote in this study, published in the New England Journal of Medicine, that, “timely and effective disclosure can enhance patient and public trust.”
Although some may disagree, it can be reasonably argued that the Air Force’s notification on Monday of the clinic’s patients “at risk” for a bloodborne viral infection a year after identifying this endoscope-reprocessing mistake is not timely.
For its part, the Air Force wrote in Monday’s press release that, “We take potential risk to patient safety very seriously and are committed to informing those under our care of any increased risk.”
Audits performed? Indication in Monday’s press release that the “at risk” patients were not told of the infection-control breach until April 2016 – almost eight years after the error began – suggests another concern:
that the clinic’s medical technicians responsible for reprocessing GI endoscopes at the clinic were not adequately trained and monitored, and their practices were not periodically audited as guidelines recommend, to confirm compliance with important infection-control standards.
Several infection-control standards recommend that technicians demonstrate endoscope-reprocessing competency “at least annually.”
In September 2015, almost six months before this Qatari clinic’s breach was identified, the federal Centers for Disease Control and Prevention (CDC) issued a health advisory entitled, “Immediate Need for Healthcare Facilities to Review Procedures for Cleaning, Disinfecting, and Sterilizing Reusable Medical Devices.
The CDC advised in this alert that, “healthcare facilities should regularly audit (monitor and document) adherence to cleaning, disinfection, sterilization, and device storage procedures.”
Whether the Qatari clinic was aware of this CDC alert, like whether its technicians were, on occasion, audited and visually observed by management to confirm compliance with reprocessing standards (this medical error’s lasting eight years notwithstanding), warrants clarification.
This CDC advisory also recommends that: “Healthcare facilities should have policies and procedures outlining facility response in the event of a recognized reprocessing error or failure.”
Whether the Qatari clinic’s delay of more than a year before informing the 135 affected patients of the potential infection risk is consistent with the Air Force’s policies and procedures regarding patient notification warrant clarification.
Lessons learned? The apparent inadequate training of this Qatari clinic’s reprocessing technicians and lacking oversight of their cleaning practices are all the more confusing, because this air base’s mistake began in 2008 near the end of the decade when, just months later in 2009, three Veterans Affairs medical centers publicized a number of similar endoscope reprocessing mistakes that placed thousands of veterans at risk for infection.
Each of these three medical facilities — located in Murfreesboro (TN), Augusta (GA), and Miami (FL) — acknowledged in 2009 that they had been improperly reprocessing flexible endoscopes, including colonoscopes and their accessories.
Weeks before this report was published, news broke in the spring of 2009 that 16 veterans exposed to potentially contaminated medical equipment at the two of these VA medical centers had tested positive for viral infections, including hepatitis.
Ten of these patients had undergone colonoscopy at the Murfreesboro VA, where three months earlier, on December 1, 2008, clinicians there had noted blood in tubing used for irrigation during the procedure.
This VA-OIG found that reusable accessories used during colonoscopy performed at this Tennessean medical center were not being properly used and reprocessed. The VA-OIG reported similar findings at the VA medical centers in Augusta and Miami.
The Murfreesboro VA facility mailed letters on February 9, 2009 – almost one year after this Qatari clinic’s breach reportedly began – to 6,387 patients notifying them of their potential exposure to HIV and the hepatitis B and viruses during colonoscopy.
In all, the VA-OIG identified instrument-reprocessing lapses at all three of these VA medical centers, resulting in its decision to notify approximately 10,000 U.S. veterans, in 2009, of their potential exposure to improperly sanitized endoscopic equipment.
The VA-OIG’s June 2009 well-publicized report heightened concerns about the risks posed by medical facilities improperly reprocessing GI endoscopes.
Warranting further investigation and clarification, it remains unclear whether clinics within the U.S. Armed Forces, including the Al Udeid Air Base, were informed of the VA-OIG’s report (or the CDC’s Sept. 2015 health advisory addressing auditing), and that the improper reprocessing of GI endoscopes could result in serious infections.
Advice that now rings with instruction and irony eight years after this air base’s reprocessing error first began in April 2008, the VA-OIG’s 2009 report recommended that:
The VA-OIG’s report added that, “Failure of medical facilities to comply on such a large scale with repeated alerts and directives suggests fundamental defects in organizational structure.”
Also, the VA medical center in Murfreesboro notified the almost six thousand “at risk” patients approximately 2 months after identifying its mistakes, much sooner than the 14 months that elapsed between the Air Force’s identification of the Al Udeid Air Base’s reprocessing breach and the notification of the “at risk” patients.
The Veterans Health Administration, the largest integrated health care system in the U.S., oversees these three VA facilities.
What about superbugs? The Air Force notified the 135 affected patients only of the risk of contracting a bloodborne virus like HIV, according to Monday’s press release.
Its decision not also to inform these patients that the Qatari clinic’s improperly reprocessed upper and lower GI endoscopes might also pose a risk of exposing patients to other types of pathogenic microorganisms including CRE may be questioned.
In addition to duodenoscopes, recent reports have linked gastroscopes to CRE infections, and some reports have linked a type of upper GI endoscope used to perform endoscopic ultrasound, or “EUS,” to infections of multidrug-resistant bacteria.
Certain EUS endoscope models, also known as linear echo-endoscopes, feature a complex design similar to duodenoscopes. Monday’s press release does not disclose whether the Al Udeid Air Base performs ERCP or EUS.
Chapman et al. (2017) sampled linear echo-endoscopes after reprocessing, reporting that a number of these endoscopes remained contaminated with “high-concern organisms” including Klebsiella pneumoniae and Escherichia coli.
After linking a deadly CRE outbreak to duodenoscopes, a hospital in Illinois in 2013 notified almost 250 patients who had undergone ERCP of the infection risk, recommending they be tested for the superbug.
Colonoscopes, too, have been found to be contaminated with concerning, multidrug resistant bacteria (although to date these lower GI endoscopes have not been directly linked to a CRE transmission).
Other types of instruments? In response to this Qatari clinic’s breach, commanders have also been directed “to complete the same review of all reusable medical instruments and devices.”
Indeed, based on the clinic’s demonstrated lack of reprocessing oversight between 2008 and 2016 — coupled with the Air Force’s directive that the reprocessing practices of other types of reusable medical equipment will now be assessed for effectiveness — it seems possible that GI endoscopes might prove not to have been the only type of instrument at the Al Udeid Air Base that might have been improperly cleaned.
The Military Health System includes the medical departments of the Air Force. Like the VHA, it is a government health program.
Recommendations
In response to this Qatari air base’s infection-control lapse, the following recommendations are provided to healthcare facilities:
- the more timely notification of “at risk” patients (e.g, within days or weeks) when an infection-control lapse that could pose a risk of serious infection is identified;
- ensuring that oversight of the cleaning and disinfection of reusable medical equipment, and notification of affected patients when an infection-control breach is identified, are consistent with the facility’s documented policies and procedures;
- the more frequent auditing and monitoring of technicians’ practices (i.e., annually, if not sooner) to ensure compliance with instrument-reprocessing standards;
- ensuring reprocessing technicians have demonstrated adequate competency for the proper cleaning and disinfection or sterilization) of reusable instruments, including upper and lower GI endoscopes; and
- staying abreast of the FDA and CDC’s published safety communications and health advisories, and of news reports to learn quickly about publicized instrument reprocessing errors, their causes and effective measures to prevent their recurrence.
Loose ends — Questions yet to be answered
Further investigation and clarification of the following issues is also recommended:
- the rationale for the Air Force not to have notified the 135 patients more timely that they could have been infected with HIV or the hepatitis B or C viruses while undergoing GI endoscopy at the clinic;
- the rationale for not notifying these patients of their potential exposure to other types of infectious pathogens such as CRE during GI endoscopy;
- the specific impetus that caused the Air Force to discover this Qatari air base’s 8-year-long breach (e.g., a routine check of the clinic’s reprocessing practices? An identified infection?). These details may provide additional insight into the cause of this clinic’s breach, and the measures the clinic adopted to prevent an endoscope-reprocessing “relapse”;
- how often management at this Qatari clinic (between April 2008 and April 2016) audited the reprocessing practices of the medical technicians to confirm their compliance with sterilization standards; and
- whether this Qatari clinic’s both oversight of endoscope-reprocessing processing and delay of more than a year before informing the 135 affected patients of the potential infection risk are consistent with the Air Force’s relevant policies and procedures.
Closing remarks, a Maryland hospital notifies patients, too
The Air Force’s press release dated June 19th suggests that important infection-prevention lessons are not being learned, and that the importance to public health of medical facilities assuring their GI endoscopes are being properly reprocessed may not be as high a priority as warranted.
Coincidentally, just last week the Largo Medical Center (in suburban Maryland) notified 23 patients of an infection risk due to their potential exposure to contaminated equipment during colonoscopy and upper GI endoscopy — the same procedures that posed the infection risk for, and is now prompting the notification of, the Qatari air base’s 135 patients.
This Largo facility is advising these 23 patients to return to the medical center for “some screening tests.” These tests presumably would evaluate the patients for viral infections, although the specific pathogens for which the patients would be screened are not disclosed in the hospital’s statement released last week.
According to this hospital, “a piece of endoscopy equipment … had a defect that might have kept it from being thoroughly disinfected. … After discovering the defect and conducting subsequent analysis, we determined that we cannot guarantee that the sterilization process was fully effective.”
The specific details of this defect, like the name of the unsafe equipment the hospital used during both upper and lower GI endoscopy, are also not disclosed in the hospital’s statement.
For its part, the hospital has concluded that “this is an extremely isolated incident” and that the infection risk is “minimal.”
Article by: Lawrence F Muscarella, PhD. Completed: June 24, 2017. Updated: June 27, 2017. LFM Healthcare Solutions, LLC. Copyright 2017. LFM Healthcare Solutions, LLC. All rights reserved.
Lawrence F Muscarella PhD is the owner of LFM Healthcare Solutions, LLC, a Pennsylvania-based quality improvement and consulting company that provides safety services for hospitals, manufacturers and the public. Email Dr. Muscarella for more details.
Tip of iceberg, as you well know, in the contaminated scope cover-up.